Diabetic foot ulcerations are a serious and potentially life-threatening complication for people living with diabetes. These wounds often develop quietly due to nerve damage or poor circulation, making them difficult to notice early and highly susceptible to infection. When left untreated, diabetic foot ulcers can escalate quickly, resulting in loss of limb or even life.
What Is a Diabetic Foot Ulcer?
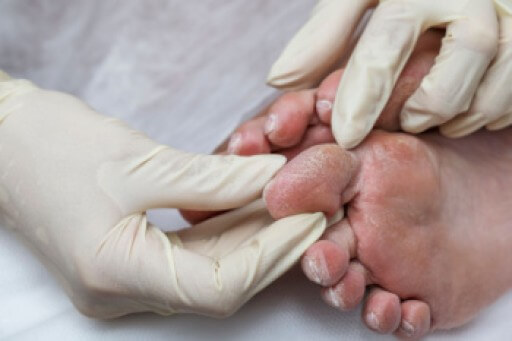
A diabetic foot ulcer is an open sore most often found on the bottom of the foot or toe. Diabetes can damage nerves and blood vessels, causing poor sensation and slower healing. For many patients, small injuries go unnoticed, and wounds do not heal as they should, raising the risk of infection
Why Are Ulcers Dangerous?
- High infection risk: Diabetes weakens immune function. Ulcers are easy targets for bacteria, making serious infections likely and sometimes spreading to bones or the bloodstream.
- Amputation risk: Over 80% of diabetes-related foot amputations begin with an untreated ulcer. When tissue dies from an advancing infection, amputation may become the only option.
- Impact on overall health: The likelihood of surviving five years after a major diabetic foot problem is lower than the average for some cancer diagnoses. Complications are often severe and long-lasting.
Preventing Diabetic Foot Complications
Understanding the progression of a foot ulcer can help patients take their daily foot checks more seriously. Often, it starts with a simple loss of feeling.
Shutterstock
Why Prevention Matters
- Reduced Sensation: Nerve damage (neuropathy) means you may not feel a pebble in your shoe or a blister forming.
- Slower Healing: Poor circulation prevents the “building blocks” of healing from reaching the wound.
- Infection Risk: A small crack in the skin can quickly become a gateway for dangerous bacteria.
Your Daily Foot Health Checklist
Use this simple routine to stay ahead of complications:
| Action | What to Look For |
| Inspect | Use a mirror to check the bottoms of your feet for redness, blisters, or cuts. |
| Protect | Never walk barefoot—even indoors. Wear moisture-wicking socks and fitted shoes. |
| Manage | Monitor your blood sugar levels daily to support your body’s natural healing. |
| Schedule | Visit WeTreatFeet Podiatry for professional nerve and circulation screenings. |
What Happens Without Treatment?
- Ulcers enlarge and deepen, increasing infection risk
- Advanced infections can result in sepsis, hospitalization, and even major surgery
- Without prompt care, limb loss or death becomes a real possibility, especially for those with other health problems.
Protecting Your Feet
- Examine feet daily for changes, cuts, or wounds—even if there’s no pain
- Don’t hesitate to ask WeTreatFeet Podiatry for regular foot exams; early detection is key to preventing complications
- Keep blood sugar well controlled and follow medical advice to slow or prevent ulcer development.
- Wear well-fitted footwear and avoid walking barefoot
- Call immediately for any new ulcer, sore spot, or skin change.

Early treatment saves limbs and lives. When in doubt, reach out to WeTreatFeet Podiatry for prompt care and expert guidance

Frequently Asked Questions: Diabetic Foot Ulcers
What is a diabetic foot ulcer?
A diabetic foot ulcer is an open sore or wound typically located on the bottom of the foot or the toes. Because diabetes often causes nerve damage and poor circulation, these wounds can develop without pain and heal much slower than a normal injury, significantly increasing the risk of infection.
Why are these ulcers considered life-threatening?
Diabetic foot ulcers are dangerous because they can escalate rapidly. Diabetes weakens the immune system, making it easier for bacteria to cause serious infections that can spread to the bone or bloodstream (sepsis). Research shows the five-year survival rate after a major diabetic foot complication is actually lower than that of some cancer diagnoses.
Can a foot ulcer lead to amputation?
Yes. In fact, over 80% of diabetes-related foot amputations begin with a single untreated ulcer. If an infection becomes too advanced or tissue dies due to poor blood flow, amputation may become the only medical option to save the patient’s life.
Why didn’t I feel the ulcer forming?
Many people with diabetes suffer from nerve damage (neuropathy), which causes a loss of sensation in the feet. This means you might not feel a blister, cut, or small injury. These small issues can quietly develop into deep ulcers because the body’s “warning system” of pain is no longer working.
How can I prevent diabetic foot complications?
Prevention starts with daily vigilance and professional care:
- Daily Inspections: Check your feet every day for cuts, redness, or skin changes.
- Proper Footwear: Always wear well-fitted shoes and avoid walking barefoot.
- Blood Sugar Management: Keep your glucose levels controlled to improve healing and nerve health.
- Professional Exams: Schedule regular check-ups with WeTreatFeet Podiatry for expert screenings.
When should I see a podiatrist?
You should call immediately if you notice any new ulcer, sore spot, or skin change—even if it doesn’t hurt. Early detection is the single most important factor in preventing limb loss and life-threatening infections.